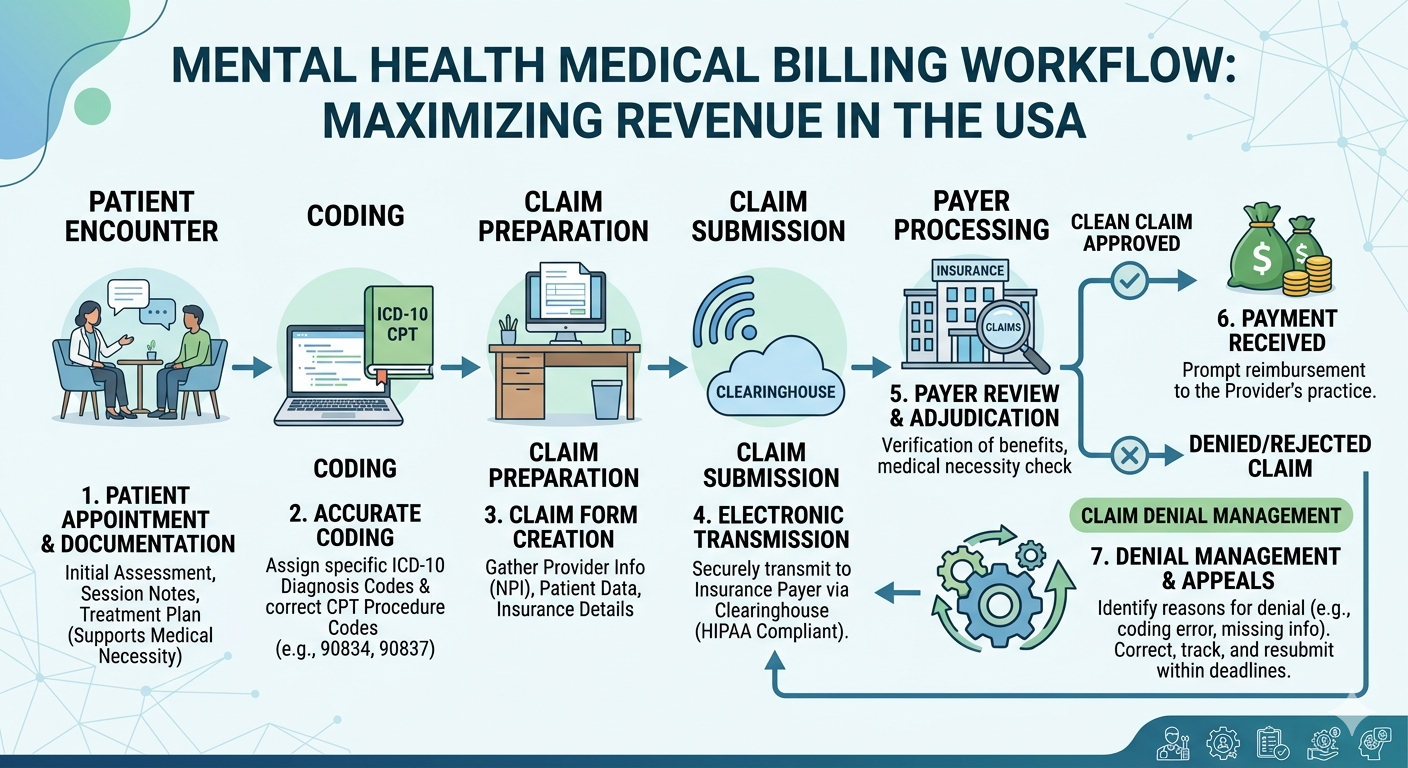
Mental health practices across the United States are expanding rapidly as more people seek professional support for conditions such as anxiety, depression, trauma, and behavioral disorders. While patient demand continues to grow, managing the financial side of a practice can be complex. Billing mental health services involves strict coding rules, payer regulations, documentation requirements, and compliance standards that many providers struggle to manage alongside patient care.
Mental health professionals such as psychiatrists, psychologists, counselors, and therapists must ensure that claims are submitted accurately and on time. Errors in coding or documentation can lead to claim denials, delayed payments, and revenue loss. As a result, many practices now rely on specialized mental health billing services to streamline their processes and maintain financial stability.
This guide explores how billing mental health works in the United States, the challenges providers face, and how professional billing support can improve efficiency and revenue.
Key Points Providers Should Know
• Mental health billing requires specialized CPT codes, modifiers, and documentation standards.
• Insurance requirements for behavioral services differ from other medical specialties.
• Incorrect coding often results in claim denials and delayed reimbursements.
• Outsourcing billing allows providers to focus on patient care rather than administrative tasks.
• Credentialing and payer enrollment play a major role in timely reimbursements.
• Medicare, Medicaid, and commercial insurance each have different billing policies.
Understanding Billing Mental Health Services in the USA
Billing mental health services is different from traditional medical billing because treatment often involves therapy sessions, long-term care plans, and specialized documentation. Providers must ensure that each claim accurately reflects the services delivered and meets payer requirements.
Medical billing for mental health typically includes services such as psychiatric evaluations, individual therapy sessions, group therapy, medication management, and telehealth consultations. Each of these services requires specific CPT codes and documentation that justify medical necessity.
Because of these complexities, many practices partner with billing companies for mental health that understand the unique requirements of behavioral health claims. These professionals ensure claims are submitted correctly, reducing denials and improving reimbursement timelines.
The Role of Mental Health Billing Companies
A professional mental health billing company helps practices manage their revenue cycle from patient registration to final payment collection. These companies employ trained specialists who understand payer policies, coding guidelines, and compliance regulations.
Mental health billing specialist companies typically handle tasks such as insurance verification, coding, claim submission, denial management, payment posting, and patient billing. Their expertise ensures that providers receive accurate reimbursements while remaining compliant with healthcare regulations.
Many providers choose a mental health billing services company because it reduces administrative stress and allows them to dedicate more time to patient care. A top mental health billing company also provides reporting tools that help practices track their financial performance and identify opportunities for improvement.
Key Services Offered by Mental Health Billing Providers
Modern mental health billing solutions cover a wide range of services that support healthcare providers throughout the revenue cycle.
Insurance Verification and Eligibility Checks
Before treatment begins, billing teams verify a patient’s insurance coverage, benefits, and authorization requirements. This step ensures that providers understand reimbursement rules and reduces the risk of claim rejection.
Coding and Claim Submission
Coding and billing for mental health services requires specialized knowledge of CPT codes related to psychotherapy, psychiatric evaluation, crisis intervention, and medication management. Accurate coding ensures claims meet payer guidelines and reduces denial rates.
Payment Posting and Reconciliation
Once insurance payments are received, billing teams update accounts, reconcile payments, and identify discrepancies that require follow-up.
Denial Management
Denied claims are analyzed to determine the reason for rejection. Billing specialists correct errors, submit appeals, and resubmit claims when necessary to recover lost revenue.
Credentialing and Payer Enrollment
Mental health billing and credentialing services ensure providers are enrolled with insurance companies and eligible to receive reimbursements. Credentialing is essential for therapists and clinics seeking to expand their patient base.
Why Many Providers Are Outsourcing Mental Health Billing
The complexity of behavioral healthcare reimbursement has led many providers to explore outsourcing mental health billing. External billing experts offer specialized knowledge and dedicated resources that in-house teams may lack.
Outsourced billing for mental health helps reduce administrative workload and ensures that claims are handled by professionals who focus exclusively on revenue cycle processes.
Outsourcing mental health billing and coding also improves claim accuracy, reduces denials, and speeds up payment cycles. Practices that partner with experienced mental health billing specialist companies often see significant improvements in their financial performance.
Benefits of outsourcing mental health billing include improved efficiency, reduced staffing costs, faster claim processing, and access to experienced billing professionals who stay updated with changing payer regulations.
Common Challenges in Billing for Mental Health Providers
Despite technological advancements, billing for mental health providers remains challenging due to regulatory complexity and frequent payer policy changes.
Documentation Requirements
Mental health services require detailed documentation that justifies the medical necessity of treatment. Incomplete or inaccurate notes can lead to denied claims.
Coding Errors
Incorrect CPT codes or missing modifiers can result in reimbursement delays. Coding for behavioral services often differs from general medical billing, requiring specialized expertise.
Insurance Policy Variations
Different insurance companies follow different reimbursement guidelines. Providers must stay updated on payer-specific rules to avoid claim rejections.
Credentialing Delays
Without proper credentialing, providers cannot bill insurance companies. Delays in payer enrollment can significantly affect revenue.
Mental Health Billing for Therapists and Clinics
Therapists, psychologists, and counselors often struggle with billing responsibilities because their primary focus is patient care. Billing for mental health therapists involves session-based claims, treatment documentation, and payer compliance.
Billing services for mental health clinics ensure that therapy sessions are accurately coded and submitted. Professional billing teams track payer guidelines and ensure that therapy sessions meet reimbursement criteria.
Many clinics rely on billing services for mental health to manage complex insurance interactions, follow up on unpaid claims, and handle patient billing inquiries.
Medicare and Mental Health Billing
Medicare plays a significant role in providing coverage for behavioral health services in the United States. Billing Medicare for mental health services requires strict adherence to CMS guidelines and documentation standards.
Providers must ensure that services are medically necessary and performed by qualified professionals. Proper coding and accurate documentation are essential to avoid audits and reimbursement issues.
Medical billing for mental health providers treating Medicare patients also involves understanding telehealth rules, therapy session limits, and eligibility requirements.
Choosing the Best Mental Health Billing Services Company
Selecting the best mental health billing services company requires careful evaluation of experience, technology, and compliance expertise.
Providers should look for companies that specialize in behavioral and mental health billing services rather than general medical billing. A best mental health billing company will understand the complexities of therapy billing, payer policies, and coding guidelines.
When comparing billing companies for mental health, providers should consider factors such as claim success rates, reporting transparency, security compliance, and customer support.
Some practices also look for a cheap outsource mental health billing company that provides cost-effective services without compromising accuracy or compliance. However, quality and experience should always be prioritized over price.
The best outsource mental health billing and coding services combine advanced billing technology with experienced professionals who understand behavioral healthcare reimbursement.
How Mental Health Billing Solutions Improve Practice Growth
Efficient mental health medical billing is essential for maintaining steady cash flow and supporting practice expansion. When billing processes run smoothly, providers can focus on patient care while ensuring their services are properly reimbursed.
Professional mental health billing services help practices reduce claim errors, increase reimbursement rates, and maintain compliance with healthcare regulations. They also provide financial insights that help clinics improve operational efficiency.
For many providers, partnering with a reliable mental health billing company is a strategic decision that allows them to scale their operations without increasing administrative workload.
Healthcare organizations such as 247 Medical Billing Services support providers with comprehensive revenue cycle solutions, including medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services. These integrated solutions help mental health practices streamline operations, improve compliance, and maintain consistent revenue growth.
Conclusion
Billing mental health services in the United States requires specialized knowledge, accurate coding, and a deep understanding of payer regulations. From therapy sessions to psychiatric evaluations, each service must be documented and billed correctly to ensure timely reimbursement.
As mental health practices continue to grow, many providers are choosing to work with professional mental health billing specialist companies that understand the complexities of behavioral healthcare reimbursement.
Whether managing billing internally or partnering with a trusted provider, investing in efficient mental health billing solutions is essential for maintaining financial stability and delivering high-quality patient care.
Frequently Asked Questions
What is billing mental health services?
Billing mental health services refers to the process of submitting insurance claims and managing reimbursements for therapy, psychiatric evaluations, medication management, and other behavioral health treatments.
Why is mental health billing different from general medical billing?
Mental health billing involves unique CPT codes, therapy session documentation, and specialized insurance guidelines that differ from traditional medical services.
Should therapists outsource mental health billing?
Many therapists choose outsourcing mental health billing to reduce administrative workload, improve claim accuracy, and ensure faster reimbursements.
What services do mental health billing companies provide?
Mental health billing companies handle insurance verification, coding, claim submission, denial management, payment posting, credentialing, and revenue cycle reporting.
How can providers choose the best mental health billing company?
Providers should evaluate experience in behavioral healthcare, claim success rates, compliance standards, reporting transparency, and the ability to handle complex billing for mental health services.