Mental health practices across the United States are experiencing rapid growth as awareness and demand for therapy and behavioral health services continue to increase. However, with this growth comes a significant administrative burden. Insurance claims, coding regulations, payer requirements, and compliance rules often create challenges for therapists, psychologists, psychiatrists, and mental health clinics.
A reliable mental health billing agency plays a critical role in helping providers manage these complex billing processes. By handling insurance claims, coding, and reimbursements, billing professionals allow clinicians to focus on patient care instead of administrative tasks.
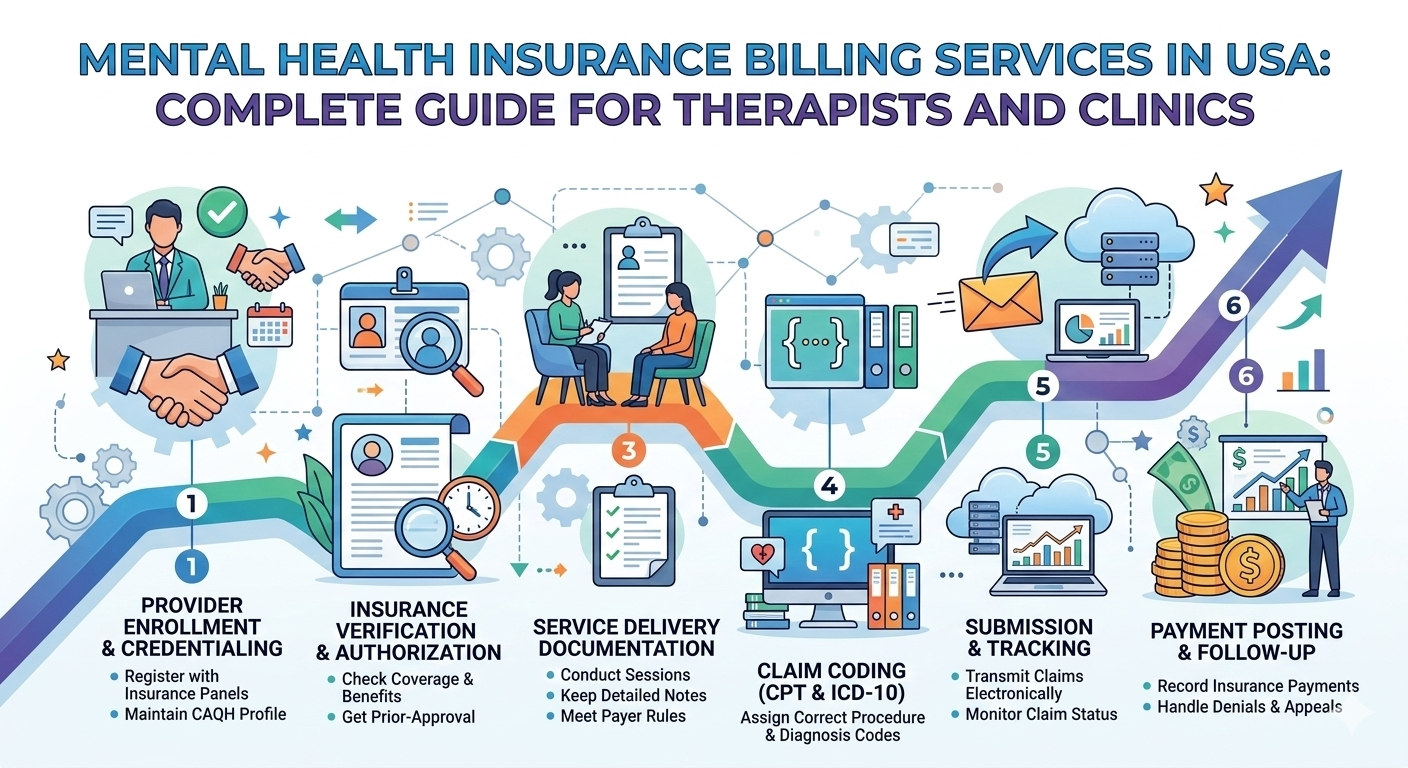
In this guide, we will explore how mental health billing works, why outsourcing is becoming popular among providers, and how to choose the best mental health billing agency in the USA.
Why Mental Health Billing Is More Complex Than Traditional Medical Billing
Mental health billing involves unique coding rules, session-based services, and insurance authorization requirements that differ from many other medical specialties. Behavioral health providers must also manage frequent documentation requirements and payer-specific regulations.
Some of the common challenges include:
-
Frequent insurance verification requirements for therapy sessions
-
Strict documentation guidelines for mental health insurance billing
-
Complex CPT and ICD coding requirements
-
Prior authorization rules for certain treatment plans
-
Delayed reimbursements due to claim errors
Because of these challenges, many clinics rely on mental health billing specialist professionals who understand payer rules and behavioral health regulations.
What Does a Mental Health Billing Agency Do?
A mental health billing services agency manages the entire billing workflow for behavioral health practices. This includes submitting claims, handling denials, verifying insurance eligibility, and ensuring accurate coding.
Typical services offered by a professional mental health billing company include:
Insurance verification and eligibility checks
Claim submission and electronic billing
Denial management and appeals
Payment posting and reconciliation
Compliance monitoring and documentation review
Financial reporting and revenue tracking
These services help ensure accurate claims submission and faster reimbursements for mental health providers.
Key Benefits of Outsourced Mental Health Billing
Many practices are choosing outsourced mental health billing to improve operational efficiency and reduce administrative stress.
Improved Revenue Collection
Working with a mental health billing provider ensures claims are submitted accurately and promptly, reducing payment delays and increasing revenue flow.
Reduced Administrative Burden
Therapists and clinical staff often spend hours managing claims and paperwork. Outsourcing billing services for mental health therapists allows providers to focus more on patient care.
Access to Billing Expertise
A mental health billing consultant or specialized billing team understands payer requirements, coding updates, and compliance regulations that many clinics struggle to manage internally.
Lower Operational Costs
Hiring and training an in-house billing department can be expensive. Mental health medical billing services outsourcing provides experienced billing professionals at a lower cost.
Better Claim Accuracy
A skilled mental health billing specialist ensures proper documentation and coding, which reduces claim denials and rejections.
Services Offered by a Mental Health Medical Billing Solution
A comprehensive mental health medical billing solution goes beyond simple claim submission. It covers the entire revenue cycle and helps practices maintain financial stability.
Insurance Verification
Before each patient visit, the billing team confirms coverage details and co-pay requirements to avoid billing errors.
Coding and Compliance
Experienced teams from a mental health billing and coding company ensure that CPT and ICD codes match clinical documentation.
Claim Submission and Tracking
Claims are submitted electronically and monitored to ensure timely processing by insurance companies.
Denial Management
When claims are denied, billing experts investigate the cause, correct errors, and resubmit claims quickly.
Accounts Receivable Management
Billing companies for mental health monitor unpaid claims and follow up with insurers to accelerate reimbursements.
Why Mental Health Providers Choose Outsourcing
The demand for outsourcing mental health billing and coding continues to grow among therapists, counselors, and behavioral health organizations.
Some key reasons providers choose a top outsource mental health billing company include:
Consistent claim follow-ups that improve collections
Dedicated billing specialists familiar with behavioral health coding
Better compliance with federal and payer regulations
Reduced staff workload and administrative overhead
Improved financial transparency through detailed reporting
Many clinics find that outsourced mental health billing improves both revenue and operational efficiency.
How to Choose the Best Mental Health Billing Agency
Selecting the best mental health billing agency requires careful evaluation. Providers should consider several factors before partnering with a billing company.
Industry Experience
Look for a mental health billing services company with proven experience handling behavioral health claims.
Dedicated Billing Experts
Top providers employ mental health billing specialist companies that focus specifically on mental health and therapy practices.
Transparent Reporting
The best mental health billing services company should provide clear financial reports and claim tracking dashboards.
Compliance and Security
Billing companies must follow HIPAA regulations and maintain secure data systems.
Customized Services
The best mental health billing company should offer flexible solutions tailored to the needs of therapists, group practices, and mental health clinics.
How a Mental Health Billing Company Improves Practice Growth
A top mental health billing company can significantly improve the financial performance of a behavioral health practice.
Higher Claim Approval Rates
Experienced teams reduce coding mistakes and documentation errors.
Faster Insurance Payments
A professional mental health billing provider follows up on claims and minimizes delays.
Improved Cash Flow
Efficient billing processes ensure consistent reimbursement cycles.
Practice Expansion
With billing operations handled by experts, providers can focus on expanding services and increasing patient capacity.
Who Can Benefit from Mental Health Billing Services
Several types of professionals rely on billing services for mental health providers.
Psychiatrists
Psychologists
Licensed therapists and counselors
Behavioral health clinics
Substance abuse treatment centers
Telehealth mental health providers
These professionals often require specialized mental health insurance billing services to manage payer-specific rules and reimbursement policies.
What Makes the Best Mental Health Billing Services
The best mental health billing services combine industry expertise, advanced technology, and dedicated revenue cycle management.
Characteristics of a top provider include:
Experienced mental health billing consultant teams
Advanced claim tracking and billing software
Efficient denial management processes
Transparent communication with providers
Continuous monitoring of payer policy updates
A professional mental health billing company helps providers maintain financial stability while ensuring compliance with healthcare regulations.
Why Partner With a Professional Mental Health Billing Company
Working with a trusted mental health medical billing services provider allows practices to streamline operations and improve financial outcomes.
A specialized mental health billing agency understands the unique needs of behavioral health professionals. By handling billing tasks, insurance claims, and compliance requirements, these agencies ensure smooth revenue cycles for mental health providers.
Many organizations now partner with the best outsource mental health billing and coding company to simplify administrative processes and maximize reimbursements.
Healthcare organizations like 247 Medical Billing Services support providers with comprehensive healthcare solutions including medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services. These services help practices maintain efficient operations and consistent financial performance.
Conclusion
Mental health providers play a crucial role in supporting emotional and psychological well-being. However, managing billing and insurance claims can create administrative challenges that reduce efficiency and revenue.
A reliable mental health billing agency helps providers navigate complex insurance requirements, reduce claim errors, and maintain a steady cash flow. From insurance verification to denial management, a specialized billing partner ensures that every claim is processed accurately.
For therapists, psychiatrists, and behavioral health clinics looking to improve financial performance and reduce administrative workload, partnering with an experienced mental health billing services company can be a strategic investment in long-term practice growth.
Frequently Asked Questions
What is a mental health billing agency?
A mental health billing agency is a specialized service provider that manages insurance claims, coding, reimbursements, and revenue cycle processes for behavioral health professionals.
Why should therapists outsource mental health billing services?
Many therapists outsource mental health billing services to reduce administrative work, improve claim accuracy, and ensure faster reimbursements from insurance companies.
How do mental health billing companies improve revenue?
Mental health billing companies improve revenue by reducing claim errors, managing denials efficiently, and ensuring proper documentation and coding.
What services are included in mental health medical billing services?
Mental health medical billing services typically include insurance verification, coding support, claim submission, denial management, payment posting, and accounts receivable follow-ups.
How do I choose the best mental health billing services company?
To choose the best mental health billing services company, evaluate their experience with behavioral health claims, compliance practices, reporting transparency, and customer support.
Is outsourcing mental health billing cost effective?
Yes, outsourced mental health billing can be cost effective because it reduces staffing costs, improves claim approval rates, and increases overall revenue collection for mental health practices.